Seizures
Seeing a child or young person having a seizure can be frightening. Most seizures do not cause serious harm. The most common type of seizure in children is a febrile convulsion. This is a seizure associated with a high temperature. This sort of seizure tends to occur in younger children.
Seizures sometimes occur without a fever (afebrile seizure). If your child has had only one afebrile seizure, it does not always mean they have epilepsy. Many children will never have another one.
First aid for a convulsive seizure:
A convulsive seizure is where the child is stiff or shaking. The information below can help you to focus when your child is having a seizure. It can help you to give first aid to keep them safe:
Do
• Stay calm
• Protect them from injury (remove harmful objects from nearby)
• Cushion or gently hold your child’s head to protect them from head injury
• Note the date and time the seizure started. If stiffness and, or jerking continues for 5 minutes or more you should call 999 for an ambulance
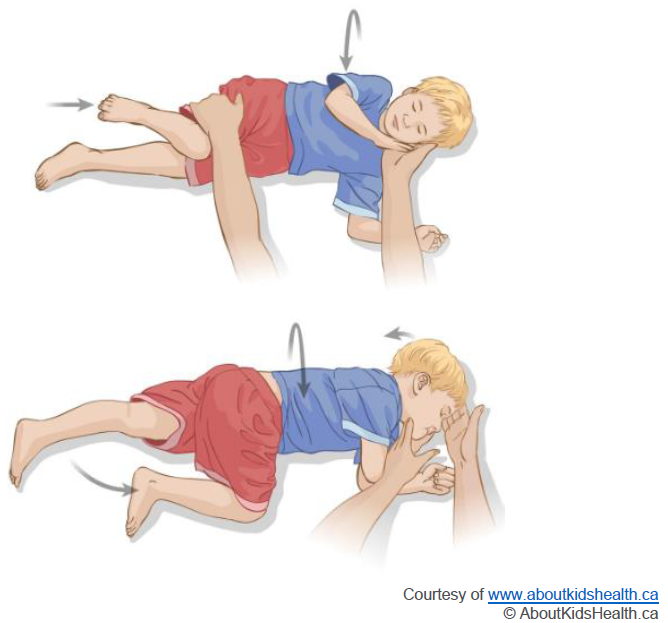
• Turn your child onto their side, into the recovery position as soon as you are able (as shown in image 1). This can help with their breathing and help if they vomit or have other types of fluid in their mouth. Some noisy breathing and slight colour change is common
• If possible, try to video the seizure on a mobile phone as it can provide a lot of useful information to your child’s doctor or nurse. Video can help confirm the type of seizure which then helps decide which tests and treatment may be needed. Try to capture the whole child in the video, say out loud what you are seeing and show how they respond to you
• Stay with your child until they are fully recovered
• Your child may be confused, drowsy or fall asleep after a seizure. Reassure them if they are confused and let them rest or sleep if they are drowsy. Make sure you keep an eye on them until they are fully recovered
Do not
• Restrain or restrict your child’s movements
• Move your child unless they are in danger
• Put anything in their mouth
• Give your child anything to eat or drink until they have fully recovered
Call 999 for an ambulance if:
• The stiffness and, or jerking continues for 5 minutes or more
• One seizure follows another before your child has fully recovered
• Your child is injured, or you are worried about their breathing
Moving a child into the recovery position:
When should you worry?
If your child has any of the following:
-
Is under 1 year of age
-
The first time your child has had a fit (seizure)
-
Has a fit that lasts longer than 5 minutes
-
They have one fit after another without being awake in between
-
They are seriously injured during the fit
-
Remain drowsy or confused more than an hour after their fit
-
Has weakness of the arms or legs, visual difficulties (double vision) or difficulty speaking after the fit has stopped
-
They have trouble breathing after the fit has stopped
-
Breathing very fast or breathing that stops or pauses
-
Working hard to breathe, drawing in of the muscles below the ribs, or noisy breathing (grunting)
-
Becomes pale, blue, mottled and/or unusually cold to touch
- Develops a rash that does not disappear with pressure (the Glass Test)
You need urgent help
Phone 999 or go to the nearest Hospital Accident and Emergency Department
If your child has any of the following:
-
Has another fit (less than 5 minutes) within the same illness
-
Breathing a bit faster than normal or working a bit harder to breathe
-
Dry skin, lips, tongue or looking pale
-
Not had a wee or wet nappy in last 12 hours
-
Poor feeding in babies (less than half of their usual amount)
-
Irritable (Unable to settle them with toys, TV, food or hugs even after their fever has come down)
-
A temperature 39°C or above in babies 3 to 6 months
-
Temperature of 38°C or above for more than 5 days or shivering with fever (rigors)
- Seems to be getting worse or if you are worried
You need to contact a doctor or nurse today
Please ring your GP surgery or call NHS 111
If symptoms persist for 4 hours or more and you have not been able to speak to either a member of staff from your GP practice or to NHS 111 staff, recheck that your child has not developed any red features
If none of the above features are present
Seizure lasting less than 5 minutes with full recovery in a child with previous febrile convulsions or known epilepsy
-
Watch them closely for any change and look out for any red or amber symptoms
-
If your child has a long term condition or disability and you are worried please contact your regular team or follow any plans that they have given you.
Additional advice is also available to young families for coping with crying of well babies.
Self care
Continue providing your child’s care at home. If you are still concerned about your child, call NHS 111
This guidance has been reviewed and adapted by healthcare professionals across West Yorkshire with consent from the Hampshire development groups.
Seizures associated with fever (febrile convulsion)
A febrile convulsion is a seizure that occurs in some children with a high temperature (fever). Although it can be extremely scary the first time you see your child have one, most of the time they are not serious. Most occur with common illnesses such as ear infections, colds and other viral infections. Full recovery with no permanent damage is usual. The main treatment is aimed at the illness that caused the fever.
Who gets them?
- They occur in about 1 in 20 children, most commonly between 6 months to 3 years of age
- They often occur on the first day of an illness associated with fever. There appears to be no connection between how high a child’s fever is and whether they have a seizure. They can occur even with mild fevers
- Most children will not have another seizure during the same illness
- 1 in 3 children who have a febrile convulsion may go on to have further febrile convulsions in the future. This is more likely if other members of the family have had febrile seizures
- Febrile convulsions are not epilepsy. Regular treatment for prevention of future seizures is usually not necessary. There is a small risk of your child developing epilepsy in the future and many parents worry about this. However, most children who have simple febrile convulsions grow out of them and do not develop epilepsy
- If your child has had a previous febrile convulsion, has a clear cause for their fever, their seizure stops quickly and they are back to normal soon after, they may be cared for at home. The first time your child has a seizure, you should call an ambulance
- Once they have been examined, if a cause is found and your child is well, it may be appropriate that they are discharged to continue recovering at home
Seizures not associated with fever (afebrile seizures):
If your child has had only one afebrile seizure, it does not always mean they have epilepsy. Some children will never have another one. In addition, children can have events that look very similar to a seizure but they are not. These include faints, tics, day dreams, sleep disorders and breath holding attacks. However, if your child has more than one seizure, they will need to investigated for possible epilepsy.
What should you do?
- When the seizure stops, you can give them paracetamol (calpol) or ibuprofen. However, there is little scientific evidence to suggest that this will stop them having a further febrile convulsion. Always follow instructions on the bottle and do not exceed daily maximum doses
- Tepid sponging is not recommended. It does not reduce fever and may cause your child discomfort
How long will the symptoms last?
- In most cases, children with simple febrile convulsions appear dazed and their eyes may roll back
- Their bodies may go stiff, their arms and legs may twitch or shake and they will become unresponsive for a few seconds. It is unusual for the febrile convulsion to last for more than 5 minutes
- Your child may be sleepy for a few minutes afterwards
Where should you seek help?
- If it is non urgent (rated in green above), speak to your local pharmacist
- If your child has any of the above features (rated in amber above), urgently contact your GP.
- For an urgent out of hours GP appointment, call NHS 111.
- You should only call 999 or go your nearest A&E department in critical or life threatening situations. (rated in red above)
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
All community pharmacies across England are required to be Healthy Living Pharmacies. This means that they are able to offer advice on a range of healthy living matters which includes eating a healthy diet. They can provide information leaflets and give parents, carers and young people more information about other organisations that might also be able to help.
Pharmacists are experts in many aspects of healthcare, and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment, and many have private consultation areas. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand. Watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
All community pharmacies across England are required to be Healthy Living Pharmacies. This means that they are able to offer advice on a range of healthy living matters which includes eating a healthy diet. They can provide information leaflets and give parents, carers and young people more information about other organisations that might also be able to help.
Pharmacists are experts in many aspects of healthcare, and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment, and many have private consultation areas. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand. Watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns, or to the Community Paediatricians, or the child and adolescent mental health services.
Contact your local Health Visiting Team:
Bradford Health Visitors or call - 01274 221223
Wakefield Health Visitors or call - 0300 373 0944
Craven Health Visitors or call - 01423 544265
Leeds Health Visitors or call - 0113 843 5683
Calderdale Health Visitors or call - 030 0304 5555 (local rate number)
Kirklees Health Visitors or call - 030 0304 5555 (local rate number)
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information about what Health Visitors do: What does a health visitor do?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns, or to the Community Paediatricians, or the child and adolescent mental health services.
Contact your local Health Visiting Team:
Bradford Health Visitors or call - 01274 221223
Wakefield Health Visitors or call - 0300 373 0944
Craven Health Visitors or call - 01423 544265
Leeds Health Visitors or call - 0113 843 5683
Calderdale Health Visitors or call - 030 0304 5555 (local rate number)
Kirklees Health Visitors or call - 030 0304 5555 (local rate number)
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information about what Health Visitors do: What does a health visitor do?
School nurses care for children and young people, aged 5 to19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and, or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse. Phone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Contact your local school nursing team:
Bradford School Nurses 01274 221203
Wakefield School Nurses (0 to 19 service) 0300 373 0944 (local rate number)
Leeds School Nurses 0113 843 5683
Calderdale School Nurses 030 3330 9974 (local rate number)
Kirklees School Nurses 0300 304 5555 (local rate number)
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
School nurses care for children and young people, aged 5 to19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and, or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse. Phone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Contact your local school nursing team:
Bradford School Nurses 01274 221203
Wakefield School Nurses (0 to 19 service) 0300 373 0944 (local rate number)
Leeds School Nurses 0113 843 5683
Calderdale School Nurses 030 3330 9974 (local rate number)
Kirklees School Nurses 0300 304 5555 (local rate number)
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
All children should be registered with a GP. Anyone in England can register for free with a GP surgery. You do not need proof of address or immigration status, ID or an NHS number.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand. Watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
All children should be registered with a GP. Anyone in England can register for free with a GP surgery. You do not need proof of address or immigration status, ID or an NHS number.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand. Watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Please note, the online version of NHS 111 is only recommended for children over the age of 5. If your child is under 5 years old, please phone 111.
NHS 111 can also direct you to your nearest urgent treatment centre (minor injuries unit or walk-in centre).
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Please note, the online version of NHS 111 is only recommended for children over the age of 5. If your child is under 5 years old, please phone 111.
NHS 111 can also direct you to your nearest urgent treatment centre (minor injuries unit or walk-in centre).
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as:
- loss of consciousness
- breathing difficulties
- severe bleeding that cannot be stopped
- major trauma such as road traffic collisions
If you’re not sure it’s an emergency, call 111 for advice.
Sound advice
A&E departments provide vital care for life-threatening emergencies, such as:
- loss of consciousness
- breathing difficulties
- severe bleeding that cannot be stopped
- major trauma such as road traffic collisions
If you’re not sure it’s an emergency, call 111 for advice.



